3er Congrés de la Bicicleta v Barceloně
| Kredity: |
Individuální rizika a prevence při cyklistice
MUDr. Dana Maňasková, 2008
Prezentace na stránkách kongresu v angličtině
Hlavní teze:
1 Nejčastější příčina vážných úrazů cyklistů je srážka s automobilem.
2 Nejčastější příčina srážek s automobilem je, že:
- řidič neviděl cyklistu - nejčastěji na křižovatkách
- řidič auta spatřil cyklistu až pozdě a nestihl zareagovat
- řidič auta špatně odhadl rychlost a vzdálenost nejčastěji
- Za šera
- V noci
- Za špatného počasí
- Ale i vlivem alkoholu a jiných drog, medikamentů či onemocnění
3 Cyklista ve svém zájmu na vozovce musí být vidět, pokud možno doslova svítit, aby ho všichni viděli již z dálky.
- Blikačky
- Reflexní vesty, obleky
- Odrazky
- Klaksony, zvonky (ev. musí být i slyšet)
- Nikdy se nespoléhat na to, že bude řidičem včas viděn
4 Mezi nejčastější příčiny vážných poranění a úmrtí cyklistů patří kraniotrauma
- Krvácení do mozku
- Pohmoždění mozku
5 Ochrana hlavy kvalitní dobře sedící přilbou je velmi důležitá. Některé studie, které se snaží svými výsledky dokázat opak, jsou vždy zatíženy nějakou závažnou metodickou chybou, která tento paradox způsobuje. Nejčastěji jde o:
- Nezohlednění rozlišnosti věkových či pohlavních kategorií cyklistů
- Nezohlednění typů poranění cyklistů - například:
- Sledování pouze čísel traumatologie, nehodnocení vážných případů, které byly hospitalizováni na jiném oddělení - např. na neurochirurgii či JIP a pod.
- Hodnocení celkových počtů ošetření, nehodnocení tíhy poranění nervového systému, následků po poranění
- Nehodnocení kvality užitých helem
- Srovnávání různých oblastí s různě vzdělanou populací a různou dostupností lékařské péče a pod.
6 Jsou lidé, kteří mají i bez úrazu při cyklistice individuálně vyšší riziko například:
- Spontánního krvácení do CNS (Warfarin, hypertenze, ateroskleroza, kuřáctví, aneuryzmata a mnoho jiných onemocnění a stavů)
- Vzniku demence (např.: vrozené dispozice k Alzheimerově chorobě a pod.)
- Vzniku epilepsie aj.
- Vzniku fraktury lebky (osteoporoza aj.)
- Vzniku kompolikující TEN a pod.
7 I nepatrná změna stavu během terapie směrem k lepšímu je pro pacienta ohromně důležitou změnou, která může rozhodovat o míře jeho limitací a soběstačnosti. I malé zmenšení traumatu mozku helmou je pro další život pacienta velmi významné. Protektivní efekt helmy je nesporný.
8 Populace stárne
- Věkem se zvyšují se rizika vzniku nehody stran cyklisty i automobilisty. Stárnoucím řidičům i cyklistům se zhoršuje:
- Zrak
- Pohotovost reakcí
- Citlivost v dolních končetinách
- Hybnost těla (krční páteř, ramena, dolní končetiny)
- Zvyšují se rizika stran poraněného - ve vyšším věku je:
- Mozek zvýšeně náchylný k traumatům, hůře se regeneruje
- Přibývající nemoci zhoršují prognózu poraněného
- Mnohá poranění vznikají snadněji
9 Zvyšuje se rychlost i počet aut a zalidněnost
- Využití kamionové dopravy
- Auta dosahují vyšších rychlostí
- Vozovky se stávají nebezpečnějšími
10 Krizová situace ve zdravotnictví a sociální sféře
- Zhoršená dostupnost zdravotní péče pro chudé pacienty
- Vyšší riziko úmrtí
- Vyšší těžších následků po úrazu
- Včetně ztráty zaměstnání, invalidity aj.
Osobní sdělení na závěr:
1 Nechcete-li nosit hlemu, jste sami proti sobě. Samozřejmě, že záleží na tom, jakou helmu si dáte na hlavu a jak si ji přivážete a ani sebelepší helma Vás při při pořádné srážce s autem nespasí.
2 Máte-li pochybnosti, zda helmu opravdu potřebujete, zkonzultujte svá indiviuální rizika stran současného zdravotního stavu a vrozených dispozic a možných následků a poté se znovu zamyslete nad otázkou helmy.
3 Hlavně nikdy nezapomeňte být na silnici viditelní na sto honů jako jedovatá mochomůrka, aby Vás žádný poloslepý pidloočka nepřehlédl - věřte, že jich bude jezdit autem čím dál víc.
4 Nejbezpečnější pro cyklistu bylo, je a vždy bude, jezdit po cyklostezkách, které jsou zcela odděleny od automobilové dopravy. A proto, kéž by takových cyklostezek bylo více, kéž by s tím noví stavitelé měst a silnic počítali více než dosud.
5 O tom, že cyklistika, obdobně jako každá jiná pohybová aktivita, je zdraví velmi prospěšná, není sporu. Jen se musí provádět za bezpečných podmínek.
Literatura:
Prezentace byla sestavena na základě rozsáhlé průřezové rešerše odborných databází zabývajících se jak otázkou cyklistiky, správné konstrukce helem, policejních zpráv o nehodovosti, tak dermografie, interny, genetiky, geriatrie, očního lékařství, neurologie, traumatologie i patologie ve vztahu ke krvácivým příhodám, rizikům pádů a zvýšené úrazovosti a úmrtnosti.
Bicycling and Individual Risk Factors
MUDr. Dana Maňasková
Czech Republic, Centrum Prevence 2000, Prague 2, Londýnská 59
1. Background:
Bicycling as an ecologic way of transport brings many healthy influences not only to cyclists themselves.Despite the fact that the main part of the responsibility for the cycling safety lies on the road and bicycle pathway engineers similarly as a safety of people living in the house lies on the architect, the doctor’s view is more concentrated on the cycling injuries.
I represent a small part of team work of specialists concerning on individualised prevention in the context of predictive genetics under the leadership of Doc. RNDr. Omar Šerý, Ph.D.
The team introduces a very unique genetic tests as well as philosophy of individually targeted prevention.As a member of the team and a doctor of a centre "Prevence 2000" I focused on the bicyclist safety and individual risks.
2. Statistics about the cyclist safety
There are thousands of articles and studies on bicycling safety. It is always necessary to consider the whole complexity of factors before making any conclusion.1) Generally, in the countries of EU, the young part of the population decreases continually - including young cyclists seen, killed or injured on the roads. There were 15% of children up to 14 years of age in the south of Czech Republic in 2006. This is 6,1% less than in 1991(Czech Statistic Office, 2008).
2) The population is getting older. The average age of drivers, cyclists and pedestrians grows. Consequences are higher portion of specific accidents, higher age of the victims of higher fatality risk while injured. The average age of hospitalised male cyclists differs in time and place a lot. For exampel: 29 years in the USA in 2005 (NHTSA, 2005) and 44 years in ČR in 2007 (Ministry of traffic in ČR, 2007).
3) There is a strong trend to develop better cars, bicycles and road surface to reach higher speeds with the risk of more fatal injuries.
4) The speed limiting strategies, alcohol examinations, medical checks of the drivers´ health and police enforcement develop differently in each country.
5) The growth of the number of motor vehicles is the common traffic complication in every bigger city that continually demands new emergency solutions.
6) With growing socioeconomic status of the society grow the safety demands on transportation system including bicycling.
7) Only in a few of the advanced countries are cycling conditions safe enough also for children and seniors. Injury statistics form these countries can show higher cycling injury rates, but completely different in spectrum of details.
8) Cycling safety in the city demands space and huge investments for its separation from the motor vehicle traffic and from pedestrians. Only several of the most progressive cities are so friendly to the cyclists.
9) Advances in emergency medicine and its organisation give higher chance to survive even worse injury. Regional differences in a medical care quality are still big.
10) Method and criterions of the study itself can lead to misleading statistic interpretations, which is a common problem.
3. Population and risk of cycling injury
The mortality of the people in the age between 1 and 40 in the EU region is mostly caused by injuries. Every life period has its spectrum of specific problems associated with injury risk including bicycling ones. There are certain population groups, that are more likely to become a victims or culprits of the traffic accidents and the safety steps should focus on them.3.1. Children
The most notable causes of children mortality in advanced countries are injuries. During child's growth the rate of home injuries drops and the rate of outdoor injuries grows, especially traffic injuries including bicycling accidents.Children under 18 years of age in the EU represent 15-24% of the population. Childhood cumulates many risk factors of fatal injuries in association with the traffic. While talking about safe bicycling in the city, there is always a question: “Is it safe enough for children?” Being a pedal-cyclist is the most-common cause of death in children over 5 years of age (Wheatley, 1989). The most of the bicycle fatalities (59%) occur before 20 years of age (Cooke, 1993). Children more easily become a victim as well as a culprit of all traffic accidents:
Behaviour: play on the road, impetuous behaviour, following of friends in dangerous activities, bicycling next to each other, crossing a road and overtaking each other without looking around , sudden entry into the road or turning off without any signalisation, poor respect or understanding the traffic rules, low rate of using a safety aids (helmets, strips, child seats) etc.
Majority (83.1%) of head injuries in children below 10 years of age occurred off-road and helmet use was lowest in this group (28.6%) (Jacobson GA, 1998).
Brain developement: Due to immature structures of the brain, children don’t have good assessment of a speed, distance, spatio-visual orientation, they have problems to differentiate between the standing and moving car, make more mistakes than adults in solving a traffic situation and have longer reacting times. 5 year old child needs circa 2-times longer time to react than an adult in the same situation. Children also have slower protective reflexes which results in a higher rate of head injury. Head injury is present in 56 % of all injuries in 1-4 year olds, but only in 19 % in 55 years and older (Henderson, 1995). Children under 10 years of age who had been riding without a helmet suffered a much higher proportion of injuries to the head (53.2% of all injuries) than older cyclists riding without a helmet (19.4 %) (Jacobson GA, 1998).
Structure of the children brain: Children have lower tolerance to impacts. The elastic deformation of the child’s skull results in more extensive diffuse brain damage than in adults (Lane, 1986). The more extensive brain injury, the higher risk of brain oedema and increase of intracranial pressure (ICP) threatens. For young children, the upper limit of normal ICP is lower than for adults (10 mmHg compared to 15mmHg). Elevations in ICP can result in cerebral ischemia and brain herniation (the movement of the brain across fixed dural structures, resulting in fatal cerebral injury) (Harrison’s principles of internal medicine, 16th edition).
Patients with severe head injuries may develop a diffuse coagulopathy due to fibrinogen depletion (result of release of tissue thromboplastin from the injured brain). A marked depletion of coagulation factors leads to higher likelihood of death (Hulka, 1996). Some studies indicate that the risk of developing coagulopathy is higher in children and that degree of coagulopathy correlates with severity of injury (Scherer, 1998).
In 32 children killed in the traffic 20 of them had skull fractures and subarachnoidal haemorrhage was present in 22 cases. There was a high percentage of damage in the corpus callosum, gliding contusions within the subcortical white matter. Intracerebral haemorrhage was relatively rare. In frontal and occipital head impacts the most injured part of the brain was corpus callosum, followed by the deep central structures and the temporal lobes, whereas injuries due to lateral impacts were more evenly distributed. Comparing of the vascular injury sector scores of children to adults suggests that children brains are more severely damaged during the same peak linear head acceleration (Gorrie, 2001).Children brain tends to have more diffuse injuries than in adults. Thraumatic intracerebral haematomas are less common in children than in adults, but early postthraumatic seizures are more common in children than in adults. Children have lower morbidity and mortality rates from thraumatic head injury compared to adults due to big regeneration capacity, but despite all that, thraumatic brain injury (TBI) is the most common cause of morbidity and mortality in children (Shepard, 2004). In 70% of children cycling fatalities head injury was present. (Nixon, 1987; Cooke, 1993)
This is also why a child who has suffered only a mild head impact should be admitted to hospital for observation. This also indicates that children's helmets should be constructed differently from adults' (Lane, 1986). The thicker the energy absorbing material of the helmet, the better protection it provides, which is especially important for children helmets. The protective level of the helmet is limited to be of a socially acceptable size (Towner, 2000). Children helmet should have thicker protective material and rounder shape. Wearing a protective helmet among children while bicycling or doing another kind of sport with the risk of head injury should be an indisputable part of a lifestyle as well as a basic hygiene is. Similarly as a newborn mortality is a marker of advance and quality of a medical care of the country, children injuries can be a marker of advance and safety of the transportation system of the country.
3.2. Men
3/4 of bicyclist crash victims are male, with a high proportion being teenagers on school trips and young adults on work trips (Henderson, 1998). Males are more severely injured in all body regions. Men also have more often fractures, sprains, dislocations and wounds. Males are 1,5 times more likely to suffer a traumatic brain injury of higher fatality (Haileyesus, 2007).Men have approximately 3-times higher mortality and 1.7 x higher morbidity compared to women and 56% of the victims with complications are men (Martin JL, 2004).Picture from: Jean A. Langlois, Sc.D., M.P.H., Wesley Rutland-Brown, M.P.H., Karen E. Thomas, M.P.H., National Center for Injury Prevention and Control, Traumatic Brain Injury in the United States, Emergency Department Visits, Hospitalisations, and Deaths, Prepared by Division of Injury Response, National Center for Injury Prevention and Control, Centers for Disease Control and Prevention, U.S. Department of Health and Human Services, January 2006 www.cdc.gov/injury

3.3. Women
The most of the hospitalised female injured bicyclists are of age 20 to 29 years.Women have significantly higher bone fragility compared to men. Due to lower skeleton resistance injuries to the neck and spinal column are twice more frequent in women than in men. Women have also much more often bruises and injuries to internal organs (including nerve roots). In single vehicle crashes with a fixed object, women had a higher risk of dying than men. If the woman is pregnant, there is also risk of losing the foetus. (Martin JL, 2004).
3.4. Seniors
This population group is one the most vulnerable ones (Topinková, 2005). It accumulates most of the risk factors for becoming a victim or culprit of a traffic accident, including that with an involvement of a cyclist.
Positives: Seniors are having more experience and carefulness. Drivers of 80 years and older had fewer rear-end crashes than drivers aged 35-54 and 70-79, and both groups of older drivers had fewer ran-off-road crashes than drivers ages 35-54 (Braitman, 2007).
Medicaments: Between 65-74 years of age 89% of the population is taking medicaments, above 75 years of age already 91- 98% of the population. Almost 60% of the seniors are not taking their medicaments according to the doctor (Topinková, 2005). Seniors are very sensitive to side effects, especially to the sedative influences on the central nervous system.
Unsuitable medicaments for the senior age are: tricycle antidepressants, barbiturates and diazepams of longer half-times, chlordiazepoxid, reserpin, methyldopa, levodopa, bromcriptin, pentazocin, meperidin, indometacin, propranolol, disopiramind, metoclopramid, spasmolytics, antipsychotics, anodynes, antihistaminics, H-2 blockers, theophyllin, some antibiotics, digoxin (Topinková, 2005; Alušík, 2001). These kinds of medicaments shouldn’t be prescribed to seniors and should be replaced by other types without negative side effects on mental functions (memory and attention).
Drop of the operating capabilities: Among the first signs of mental decline are the loss of ability to perform complex activity (driving a car), more easily disturbed attention, longer reacting times, lower ability to learn new things etc. Drivers over 80 predominantly failed to see or detect the other vehicle. Drivers aged 70-79 made more evaluation errors - seeing another vehicle but misjudging whether there was adequate time to proceed. Crashes where drivers failed to yield the right-of-way increased with age and occurred mostly at stop sign-controlled intersections, generally when drivers were turning left (right side driving) (Bratiman, 2007).
Mental functions: Light confusion to heavy pseudementia can be more easily caused by dehydration or common infection. There is 3-7% of the population above 65 years of age affected by dementia, 15% at 75 years of age, and 20-40% above 80 years of age (Topinková, 2005).
Perception: Vision and hearing decline in senior population is another high risk factor of traffic accidents.
Polymorbidity: Most of the seniors suffer from osteoporosis, osteoarthritis (20,6% above 60 years), atherosclerosis (91% above 65 years of age), hypertension (50% above 60 years in year 1996 with an increasing trend), diabetes mellitus (16,6% above 60 in 1996), vessel defects of the brain (6,1% in 1996 in the people above 60)etc. (Topinková, 2005). All these conditions are risk factors for brain injury, fatal complications and worse prognosis while injured.
Fatality: Fatality risk for 50-64 year old bicyclists was 3.5 times that of bicyclists 5-15 years of age (Henderson, 1995). The fatality of traumatic brain injury rate increased from 20% in childhood to 71% over 75-year-old (Javouhey, 1969). The average age of cyclists who died in hospital is 56,1 years. The counted risk of a fatal injury or death per km of the cyclists was highest for the ages 30-39 and over 65 (Neklapil, 2007).
Table from: Jean A. Langlois, Sc.D., M.P.H., Wesley Rutland-Brown, M.P.H., Karen E. Thomas, M.P.H., National Center for Injury Prevention and Control, Traumatic Brain Injury in the United States, Emergency Department Visits, Hospitalizations, and Deaths, Prepared by Division of Injury Response, National Center for Injury Prevention and Control, Centers for Disease Control and Prevention, U.S. Department of Health and Human Services, January 2006 www.cdc.gov/injury

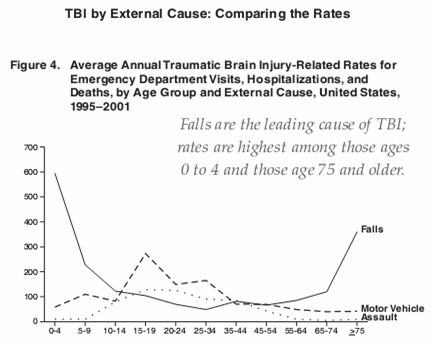
Falls: 20-30% of the seniors aged 65-69 and 50% of seniors above 85 years suffer an injury (osteoporotic fracture, traumatic brain injury etc.) in one year because of a fall (Topinková, 2005). Falls are the leading cause of traumatic brain injury. The highest rates of TBI are in children up to 4 years and seniors of 75 years and older (NCIPC, 2007).
Bicycling routes projected as a common space with pedestrians are associated wit higher rate of cyclist-pedestrian collisions and higher rate of senior pedestrian falls with fractures and TBIs, especially in females.
Due to the fact that our population is getting older, all the preventive steps must take into account all possible problems of higher age. In 1950, there was 8,3% of people over 65 years in the Czech Republic and in 2000 it's already 13,9%. It is estimated that there will be 23,1% of people over 65 years of age in ČR in 2025.
Senior cyclists should be more cautious, well informed about special risks of their illnesses and use proper helmets while cycling. Health and the quality of life and of seniors are partly given by the whole life style and partly by genetic predispositions to different diseases. Many of these predispositions can be detected by DNA tests and individually targeted prevention can be started before a disease can develop or progress (Šerý, 2007).
Picture from: Jean A. Langlois, Sc.D., M.P.H., Wesley Rutland-Brown, M.P.H., Karen E. Thomas, M.P.H., National Center for Injury Prevention and Control, Traumatic Brain Injury in the United States, Emergency Department Visits, Hospitalizations, and Deaths, Prepared by Division of Injury Response, National Center for Injury Prevention and Control, Centers for Disease Control and Prevention, U.S. Department of Health and Human Services, January 2006 www.cdc.gov/injury
4. Risk factors of traffic accidents with involvement of cyclists
The worst type of the cyclist collision is an impact of the motor vehicle with the highest rates of fatality, mostly due to head injury (Praslow, 2005) and the fear from the impact with a motor vehicle is one of the most substantial reasons of little use of a bicycle as a mean of transport.
4.1. Cognitive skills:
Attention, memory, visual processing and executive skills are the key points in the most of traffic accidents. In the base of all accidents stands a drop of vigilance, when the other participant is not seen till the last moment. Second most often cause of accident are unjustified expectations about the behaviour of others. In 37% of collisions, neither driver nor cyclist realized the danger or had time to yield. In the remaining collisions, the driver (27%), the cyclist (24%) or both (12%) did something to advert the accident (Räsänen, 1998).
Car drivers did not see the bicycle until immediately before the collision even though the bicycle must have been clearly visible. "Looked-but-failed-to-see" events do occur, especially in experienced drivers and with a higher rate if another car is present (Herslund, 2003). The probability of overlooking a cyclist by a driver of a motor vehicle grows with the liveliness of the traffic, especially in rush hours, by impaired visibility, impaired visual skills of the driver, alcohol in blood and other attention disturbances (Wilson, 2003-2005). The drivers aged 35-54 also tended to make search errors, but theirs were more often due to distraction (Braitman, 2007).
Frequent accident type of collisions between cyclists and cars is a driver turning right and a bicycle coming from the driver's right along a cycle track in 5% of all the cyclist accidents on the road (Wilson, 2003-2005). Drivers turning right hit cyclists because they looked left for cars during the critical phase. Only 11% of drivers noticed the cyclist before impact. In these cases, 68% of cyclists noticed the driver before the accident, and 92% of those who noticed believed the driver would give way as required by law. Visual scanning strategy which concentrates on detection of more frequent and major dangers occasions can ignore and may even mask visual information on less frequent dangers. The drivers turning right scanned the right leg of the T-intersection less frequently and later than those turning left (Summala H., 1996).
The most often driving offence of the cyclists and motorists leading to the accident is entering the crossroad on the red light (Wilson, 2003-2005), inappropriate way of the ride of the cyclists and not giving a way. In slightly more than 50 % of the accidents the drivers of the motor vehicles were the culprits (Police ČR, 2004).
Another risky situation is overtaking a cyclist by a motor vehicle on the road without road lines marking a bicycling space with wrong assessment of the space by the motorist (4,7 % of all the cycling accidents on the road), especially by impaired visibility at night, sunset and bad weather. Time of injury peak is in the late afternoon and early evening and remains constant across the week (Wilson, 2003-2005).
The cyclist should never expect, that the driver of motor vehicle sees him, should respect driving rules and use all reachable aids to enhance his visibility. Independently of a study and its origin, the best prevention results are being achieved by a complete separation of the bicycling routes from a motor vehicle transport.
4.2. Alcohol
The intoxicated cyclists more often sustained injuries at night time, at the weekend, on their way to or from a party or a pub/restaurant with higher rate of head and face injury. They cycled less during the year, had bicycles without a hand-brakes or gears and less often wore a helmet. Ethanol was significantly more common among males, whereas positive benzodiazepine tests were more frequent in females (Kurzthaler, 2003), the similar conclusions were made in ČR. (Mravcík, 2007; Mraček, 2004). Alcohol consumption among the cyclists is still high, but due to more strict traffic rules and controls there is a slow decline in the last years (ČR).
A cyclist under the influence of the alcohol has lowered ability of contemplation, lowered balance, propriomotoric and defence reflexes with higher risk of falls, head and brain thrauma. Brain vasodilatation due to alcohol intoxication is a risk factor of intracranial haematoma and bleeding complications.
Sedative effect of the alcohol on the central nervous system is stronger in people with depression and anxiety, or when combined with sedating medicaments as benzodiazepines, barbiturates, tricycle antidepressants etc. The effect of the alcohol is stronger in women, because of missing alcoholdehydrogenases in the wall of the stomach, smaller liver and less volume of blood. It’s possible to test DNA polymorphisms of liver enzymes and predict the individual speed of alcohol degradation.
The cyclist and the driver of motor vehicle should know well the metabolisms of the alcohol and never drive under its influence. The cyclist should know the local feasts and avoid motor vehicle traffic, especially in the evening hours. If the cyclist is riding under the influence of the alcohol, he should wear a helmet, reflexive clothes, as many as possible of lights, mobile phone, avoid the roads of motor traffic and never ride alone because of very high risk of accidents.
4.3. Psychotropic drugs
Rate of psychotropic drugs other than alcohol in blood of all killed cyclists was 7.2%. Benzodiazepines were found most frequently (3.6%), followed by cannabis (2.2%), and stimulants (1.7% of the samples). Dead cyclists with positive medicament tests were significantly older than negatives. (Mravcík, 2007). The most commonly detected benzodiazepine was diazepam (Kurzthaler, 2003).
Approximately 2/3 of population suffers form dysthymias, mild depressions or insomnias. Many of them are never diagnosed and a big part of those, who are diagnosed by a doctor, never see a psychiatrist and receive benzodiazepines instead of modern medicaments without central nervous system inhibitory side effects. Especially sensitive are seniors.
4.4. Metabolic disorders
Condition with significantly lowered attention and capability to react properly is for example hypoglycaemia of any origin. Diabetics on insulin therapy are in danger, especially if using drugs that can mask the first signs of growing hypoglycaemia: beta-blockers, ACE-inhibitors, octreotid or alcohol. Nondependent diabetics on insulin can develop hypoglycaemia when combining oral antidiabetics with drugs that stimulate insulin secretion: acetylsalicylate acid, co-trimoxazol, chinin, chinidin, disopyramid, sympatomimetics or alcohol. Cyclist with diabetes should be well educated about the proper doses of insulin and drug effects while bicycling, have something sweet and diabetic card always with.
Second very common, but less dramatic metabolic disorder with lowered attention and longer reacting times is a hypothyroidism. It occurs more frequent in women, especially older women and during winter months. Many of them are not diagnosed. Regularly screenings and an adequate therapy are necessary. Hypothyroidism might be associated with traffic accidents and cycling injury too.
4.5. Neurological disorders
Worsened capability to drive a motor vehicle or bicycle occurs due to many of the neurological or psychiatric conditions.
As already mentioned, fall is very common case of fatal injury in seniors. Easier loss of balance and falling off the bicycle can be the first sign of illness. Almost 50% of the seniors above 65 years of age suffer from vertigo.
Vertigo can be caused by labyrintitis, morbus Meniére, vessel diseases, herpes zoster oticus, benign position vertigo, brain tumours (neurinomas), meningoencephalitis, disorders of the sight, ictus, brain hypoperfusion, cerebrovascular insufficiency, cocaine, migraines, hearth insufficiency, arrhythmias, metabolic disorders, hypertension encephalopathy, higher grade of anaemia, dehydration, medicaments (aminoglyskosid antibiotics, cis platinum, loop diuretics, antihypertensives, antiepileptics, psychopharmacologic medication, amiodaron, methotrexate, anticoagulants) (Topinková, 2005).
Cyclists suffering from named conditions should choose easy terrain, avoid sharing the roads with the motor vehicles and of course, wear an appropriate helmet. Another help can be the use of a tri-cycle instead of bicycle.
At the end of the very long list of all neuropsychiatric disorders that are limiting the ability and safety of driving a car or bicycle stands a new group of detectable DNA polymorphisms that are associated with longer reaction times in healthy individuals (Krabbendama, 2006), attention disorders (Šerý, 2007; Reimera, 2006), “risk-taking genes” or “warrior genes“ predisposing a person to more hazardous behaviour (Krabbendama, 2003), similarly as infection by a common parasite Toxoplasma gondii (Flegr, 2002).
4.6. Vision and traffic accidents with involvement of bicyclist
Those older drivers with a visual attention disorder or poor scores on a mental status test had 3-4 times more accidents (of any type) and 15 times more intersection accidents than those with good test scores (Owsley, 1991). "On-the-Spot" accident investigations have confirmed that driver’s perception errors are a major contributory factor to accidents (Hills, 1980).The rapid fall in visual acuity with angular distance from the centre of vision presents particular problems, giving special significance to eye-movement and visual search especially in drivers using dioptric glasses. Physical or psychophysical restrictions of visibility can lead to the "looked, but failed to see" type of accident. The driver is quite often operating beyond his visual or perceptual capabilities in a number of key driving situations, including overtaking, joining or crossing a high-speed road, and a number of night time situations. "Expectancy", based on experience has a profound influence on driver´s perception and assessment of risk (Hills, 1980).
Cataract declines night vision, impairs contrast sensitivity, increases adjusting time of the changes in lightness and fine details. Cataract elevates at-fault crash risk among older drivers, even when present in only one eye. Cataract is a leading cause of vision impairment in older adults, affecting almost half of those older than 75 and may occur already at 40 years of age (Hills, 1980). There are several known and commonly used medicaments that can cause or impair the cataract: Amiodarone, corticosteroids, tetracyclines, salts of gold, chlorpromazine, pravastatin (Zagaria, 2007). Other known causes of the cataract are inborn predispositions, eye injuries, high age, sun radiance, smoking, diabetes mellitus, chronic inflammation with high oxidative stress and other metabolic disorders. Cataract is a second most frequent cause of senior blindness (Topinková, 2005).
Dark adaptation decrease is often referred after laser dioptric corrections of the cornea.
Visual field in the horizontal line usually decreases from 170 degrees in young adults to 140 degrees in 50-year-olds. Deficits of peripheral vision have been implicated as a major cause of automobile accidents involving drivers of advanced age with two time higher collision rates (Hills BL., 1980).
Glaucoma often destroys the field of vision if intraocular pressure is higher than 21mmHg which causes atrophy of the optical nerve. Glaucoma affects almost 5-7% of the seniors.
Other causes of limited visual field are for example: retinal abruption, retinal degeneration, diabetic retinopathy, retino-vascular disorders: vasculitis, arterial occlusion, vein occlusion, ischemia, amaurosis fugax, occipital lobe stroke, etc.
Age related macular degeneration affects 11% of the population aged 65-74 years and belongs among the most often causes of senior blindness (Topinková, 2005). More than 50% of the drivers in the makular degeneration study reported that due to the age related macular degeneration have difficulty with driving or don’t not drive at all at night, during rush hour or in heavy traffic areas, in the rain, on freeways or interstate highways (Kitchin, 2005).
After 45 years of age, everybody should be annually checked by an ophthalmologist. Today, some of the predispositions to the age related macular degeneration can be tested - for example associated polymorphisms of the PLEKHA, CFHR2 and ARMS genes which play important role in development and progression of the age related macular degeneration. If a person is a carrier of these mutations, should be supervised by the ophthalmologist, use antioxidants, control glycaemias if diabetes is present, and shouldn’t smoke to prevent the disease (Šerý et al., 2007).
As colour vision declines with the age the risk of traffic accidents increases. Colour blindness is usually completely inborn condition. Some gene mutation has been associated with colour discrimination impairment in the alcoholics (Šerý, 2008).
5. Bicycling injury
Nowadays, injuries of very high energy levels can be survived, but when the safety limits are exceeded immediate death is more common. Velocity of 6m/s (21,6 km/h) is considered to be limit speed of fatal injuries. Velocity of 16m/s (57,6 km/h) is associated with 50% risk of death. Impacts occurring in 42 m/s (151,2km/h) or higher speed are nearly 100% fatal (Vorel, 1999). Risk factors for more serious cycling injury are collision with a motor vehicle, self reported speed > 15 mph, age < 6 years or > 39 years, male sex or happened after dark (Rivara, 1997).
5.1. Injury of the head and brain
Above 80% of the hospital admissions in the USA are due to principal diagnosis of a brain contusion or internal head injury (Henderson, 1995). Almost 100% (Mraček, 2004), 90% (Soori, 2002), 80% (Henderson, 1995), 75% (Frič, 2007) of the cycling fatalities were due to head trauma and the most common surgery was decompressive craniotomy and plastics of the frontal skull hole. Hospitalised bicyclists with head injury are 20 times more likely to die as those without. (Haileyesus, 2007).
5.1.1. Concussion cerebral
Concussion cerebral is a light injury of a brain without anatomic correlate with presence of disrupted neuronal functions and EEG changes of brain activity, which normalise soon.
5.1.2. Brain contusion
In more than 1/3 of head injury is a primary diagnosis contusion and it is one of the most often cycling injuries of the head.
Contusion is caused by the movement of the brain inside the skull during the rapid deceleration after the impact of the head. CT or MRI scans show nonhomogenous cortical and subcortical petechias with a surrounding brain oedema in the localisation of “pa coup” and “par countre-coup” or a small subarachnoidal bleedings. In 3% of the brain contusions intracranial haemorrhages are present.
There are temporarily remaining changes in EEG brain activity of the reticular formation (structures activating upper mid brain). Considered cause is rotation of the brain hemispheres which are tightly connected to the brain stem during the impact of the head. This is a reason, why the cycling helmet should have the surface as smooth and symmetric as possible.
Among the brain contusion symptoms like short loss of memory, sweating and vomiting is the risk of developing hearth arrhythmias. If a cyclist has impaired heart electricity conduction (seniors after cardiac infarction or young people with inborn predispositions as WPW syndrome etc.) there is a higher risk of malignant arrhythmia and sudden death. Symptoms of the brain contusion usually subside soon.
In the brain tissue damaged by the contusion, ATP depletion with disruption of haematoencephalic barrier develops. This kind of lesion with vast consequences is more expressed in people with less production of ATP in mitochondrias due to mitochondrial DNA damages by chronically higher load of oxidation stress (senior age, mild hypoxia due to lower lung, heart or blood functions, chronic infections, alcoholism, cigarette smoking etc.), heavy acute free radical stress in anamnesis (high dose actinotherapy, chemotherapy, longer resuscitation, sepsis, intoxication by mitochondrial or respiration targeted poisons, etc.) or inborn mutations associated with lower mitochondrial function reserve.
Cyclists having a relative suffering from Alzheimer disease may have genetic predisposition to Alzheimer disease. Predictive medicine offers genetic tests on predispositions to Alzheimer disease (Šerý, 2008). There are several known mutations strongly associated to Alzheimer disease, for example ApoE4 allele. This polymorphism means a lower neuronal ability of regeneration, worse prognosis with more consequences due to brain injury. There are many other genes associated to the Alzheimer disease. A person with the risk of Alzheimer disease should protect his brain properly, avoid all sports with a danger of head impacts (box, etc.) and wear protective helmet while bicycling.
When released into the home care after a brain injury, there are several possibilities how to support recovery of the neuronal functions: enough of sleep, lecithins supply (glycerol core with phosphatidylcholins as a precursors of acetylcholine and necessary elements of the cell membranes) especially those from soya with appropriate fatty acids. Lecithins can be used in doses of tens of grams a day. Already one dose of lecithin was shown to improve memory functions in healthy adults. There is supposed preventive influence too. Phosphatidylcholins, phosphatidilserins, vitamin E, C, B12, B6, folate, reduced glutathione, green tea, curcumin, biomine, tryptophan, tyrosine, bifurcated amino acids, alpha lipoic and linoleic acid ( ALA ), docosahexaenoic acid (DHA), Vinpocetine, Piracetam, Hydergine, policosanol, pregnenolone, DHEA, amino guanidine, coenzyme Q, Gingko Biloba extracts, CDP-Cholin, fruit and vegetable antioxidants are another substances frequently studied as neuronal protective factors (Anderson, 2007). Factor that should be avoided is for example natrium glutamate (Chinese kitchen) because of slight neurotoxicity that can worsen a neuronal regeneration. If the serum cholesterol is higher, medicaments of statin group should be used. If necessary to relieve from pain, nonsteroid antirevmatics as indometacine or ibuprofen should be preferred (associated with lower rate of Alzheimer disease).
5.1.3. Diffuse axonal injury- DAI
Diffuse injuries of the brain consist of oedema, contusion and diffuse axonal injury (DAI). The axons are being disrupted by stretch or cut (rotation) forces between the different structures of the brain by the swift deceleration of the head in the localisation of corpus callosum and dorsolateral pons. The worst consequence of small haemorrhages, ischemic changes and DAI in the midbrain or thalamus is a persistent coma, a vegetative state (Harrison’s principles of internal medicine, 16th edition).
5.1.4. Intracranial bleeding
Intracranial bleeding is one of the very frequent complications of head injury, but it can develop also spontaneously without any injury. There are many risk factors and conditions of developing a spontaneous brain haemorrhage. Especially these people have a high risk of intracranial bleeding while injured.
The risk factors are: high blood pressure, amyloidal degeneration of the vessels (often in seniors), other vessel degenerations (atherosclerosis, macro- and microangiopathias in diabetics, etc.), inborn lower quality of the collagens (Ehlers-Dunlos syndrome, osteogenesis imperfecta, vessel aneurysms, etc.), brain haemorrhage in the relatives, acute infectious diseases, infectious diseases of the brain, syphilis, autoimmune diseases with a vascular involvement, smoking (highest rate of haemorrhages occur within the 3 hours after finishing a cigarette) (Kalita, 2006), cocaine, amphetamines, atrial fibrillation, glucocorticoid high dose therapy, hypoxia (lung or hearth diseases), hypercholesterolemia, deficiency of vitamin C or B12, obesity, dehydration, higher intake of natrium, alcohol, protein malnutrition, chemotherapy, actinotherapy of the head, coagulation changes with lower blood clothing like thrombocytopenia (acute HIV infection, hepatitis C (Karibe, 2001), autoimmune disorders with destruction of thrombocytes, use of medicaments like chinine, sulphonamides, heparins, cytostatics, salts of gold, diclofenac, sulfathiazole, co-trimoxazol, vancomicine, piperacilin, prokainamid, methyldopa, thiazid diuretics, carbamazepine, ranitidine, estrogens, danazol, etc.), lowered function of thrombocytes, haemophilias, low prothrombine (after surgery, insufficiency of vitamin K during use of broad-spectrum antibiotics like cefoperazon etc.), use of anticoagulants (cumarine derivates, acetylsalicylates, heparins, ticlopidine, IIb/IIa inhibitors), etc. (Alušík, 2001).
Higher fragility of the bone and brain tissue, lower homoeostasis regulation capacity with lower brain tolerance of hypoxia are another risk factors for higher extend of brain injury, intracerebral bleeding and fatality of the injury in the seniors. Any sort of prevention aid, that can help to lower the impact of the head, is of high significance in such conditions.
5.1.4.1. Epidural haematoma
Epidural haematoma also occurs very frequently in the cyclist head injury - up to 10% of the severe head injuries. Epidural haematomas are less associated with cortical brain damage, but develop more rapidly then the subdural haematomas (Harrison’s principles of internal medicine, 16th edition).
5.1.4.2. Subdural haemorrhage
10 % of the hospitalised cyclists died and the cause of death in most of he cases was brain contusion with acute subdural haematoma (Mraček, 2004). In 1/3 of the acute subdural haemorrhage cases, there is “lucid interval” before the coma develops. Acute subdural haematoma does not need to be caused by a great violence. Whiplash mechanism is fully sufficient, especially in the elderly (vessel fragility and degeneration, dehydration, brain atrophy, anticoagulant therapy, etc.). Subacute subdural haematomas may develop days or weeks. In chronic subdural haematomas 20-30% of the patients recall no head injury, because the causative injury may be trivial and often forgotten in the time of symptoms (Harrison’s principles of internal medicine, 16th edition).
5.1.4.3. Subarachnoidal bleeding
Subarachnoidal bleeding (SAH) due to head deceleration trauma is also often. Risk factors for SAH include: hypertension, cigarette smoking, and family history of a primary relative with a SAH (4% risk). Other risk factors include age (The incidence peaks between the ages of 40 and 60.), gender (women in 60% of all cases), race (African Americans have nearly twice the risk as Caucasians of SAH, but also of TBI). The risk of aneurysm rupture depends on its size. Cigarettes and alcohol abuse have been shown to increase aneurysm rupture (Anderson, 2007). Children have constitutionally wider subarachnoidal space and seniors often suffer from dehydration and brain atrophy which also leads to wider subarachnoidal space with more stretched subarachnoidal bridging arteries in a higher risk of damage by head commotion.
5.1.4.4. Intracerebral bleeding
Rotational acceleration of the hemispheres threatens by intracranial haemorrhage in the location of the basal ganglia and surrounding structures, especially in seniors (often present vascular amyloidosis) and in the individuals with impaired coagulation of the blood. Fatal bleeding can occur even a several days after the injury (Harrison’s principles of internal medicine, 16th edition).
5.1.5. Complications and consequences of the head injury
There are many neurological complications of TBI which include focal neurological deficits, global neurological deficits, arterial transactions, thromboembolic phenomena, posttraumatic aneurysms, dissections, and carotid-cavernous fistulae, hydrocephalus, vascular injuries, infections, dysfunction of cranial nerves, etc.(Shepard, 2004).
Posttraumatic seizures are frequent complications of TBI. Early seizures occur within 24 hours of the initial injury, intermediate seizures occur 1-7 days following injury, and late seizures occur more than 7 days after the initial injury. Posttraumatic seizures are very common in those with a penetrating cerebral injury, and late seizures occur almost in 50% of these patients. Superficial cortical scars from contusions are highly epileptogenic and may manifest even many years after trauma. The majority of convulsions occur within the 5 years after injury. Epilepsy develops in 2% after a mild trauma but in the 17% of the individuals with brain contusions with subdural haematomas and prolonged time of loss of consciousness.
Slightly more than 2/3 of the cases after brain trauma will probably have no sequel one year after their accident, 30.4% will probably have minor or moderate disability, and 0.7% will have serious to total disability (and, for the record, 1.2% will die) (Shepard, 2004). It depends a lot on the brain injury extension, predisposing conditions and genetic factors of the individual if and which kind of complication will develop.
5.2. Fractures
5.2.1. Injury of the spine and spinal cord
Less than <5% of head-injured patients had cervical spine injury. Spine injury must always be suspected in presence of head trauma (Bucholz, 1983). An altered state of consciousness secondary to head injury or intoxication may obscure diagnosis of a cervical spine injury. Severe head injury and skull base fractures were more frequent with upper cervical injuries (Iida, 1999). There is a slightly higher risk for women and elderly because of higher bone fragility and higher rate of osteoporosis. Only several studies provided neck injury results as unfavourable to helmets with a summary estimate of 1.36 (1.00, 1.86) but helmets currently in use weigh less than those at the time of the study (Attewell, 2001)
5.2.2. Femoral neck fractures
There is high population risk of fractures due to osteopenia, osteoporosis and many other inborn or acquired conditions with higher bone fragility. Femoral neck fractures in elderly occur most commonly after minor falls or twisting injuries, especially in women. The risk of a feet slippage off the pedal is lowered by use of binding-type pedals, but their use is inappropriate, if bone fragility is present, because of very high femoral neck fractures risk when falling on side (Slootmans, 1995).
The long list of risk factors for higher bone fragility and the list of symptoms of latent osteoporosis exceed the scope of this article.
5.3. Injury of the soft tissues
5.3.1. Thrombosis
Injuries of the extremities are very often in cycling. Severe contusions of leg, fracture, longer stay in bed together with the possible dehydration of the cyclist are the risk factors of deep venous thrombosis which can cause pulmonary embolism. Approximately 3-7% of the European population carries Leiden mutation, which is one of the most common genetic risks for thrombosis. The genetics tests are available. A person knowing that he is a carrier of Leiden mutation should wear this information with his identification cards and inform the doctor every time about his special need of thrombosis prophylaxis.
5.3.2. Infection
The absence of infectious disease belongs among the common safety terms while planning a surgery. If a cyclist who sustains a severe injury has been suffering from an infectious disease (mostly of the respiratory tract) has much higher risk of developing a complications as pneumonia, abscess formation or a sepsis. Pneumonia itself has 15% mortality in seniors (over 65 years of age) and causes up to 90% of all senior deaths (Topinková, 2005). The risk factors of severe infectious complications involve all conditions with weakened immunity and again, cumulate in the seniors: lung diseases, chronic heart insufficiency, malnutrition, diabetes mellitus, pneumonia in the past, gastroaesophageal reflux, immunosuppressive therapy, actinotherapy, glucocorticoids, chemotherapy, stomach antacids, alcoholisms, smoking, etc.
There are also known gene mutations involved in immunity system regulation that are associated with higher risk of sepsis and mortality. These tests are available today, too.
The cyclists, especially those with genetic predisposition for sepsis, should avoid bicycling while suffering from acute infections.
In case of acute or chronic sinusitis, there is high risk of intracranial infection, when the fracture of the skull crosses the sinuses. Penetrating cerebral injuries and open depressed skull fractures have also increased number of intracranial infections (Shepard, 2004), which is another argument supporting use of helmets.
5.3.3. Pneumothorax
A tension pneumothorax is a life-threatening condition that occurs when the air in the pleural space is under pressure, displacing mediastinal structures and compromising cardiopulmonary function. It is a serious complication of thoracic trauma, and it has been described in 1 in 5 patients that survive major trauma. Pneumothorax may occur also spontaneously, especially in the setting of lung disease. The risk factors of pneumothorax are: asthma, COPD, smoking, alpha 1 antitripsin deficiency (genetic disorder), chronic cough and emphysema (genetic predispositions). Besides that these individuals are more sensitive to the motor vehicle air pollution, their lungs are more mechanically endangered in case of collision with motor vehicle.
5.3.4. Hollow organs
The injury of hollow organs during the impact is more often, if not empty and while having weakened wall: full urinary bladder, gastro-duodenal ulcers, diverticulosis etc.
5.3.5. Healing of wounds
There are certain rules in healing the wounds specific for every kind of tissue, but generally, there is a need to promote the blood circulation, lower the infection, support the immune system, cell proliferation, collagen production and antioxidant capacity. There are positive reports on supplementation with vitamin C, E, A, zinc, glutathione, proteins etc.
The use of hydrocolloid gels as a surface bandage gave better results than use of standard tulle gauze (shorter healing time, smaller risks of infection, more pain relief and higher comfort) (Hermans, 1991).
Cyclist should always have a small bottle of disinfection for the case of small erosions (Iodisol, Bethadine etc.) and plaster to avoid wound infection. Every cyclists should also certainly pass a regularly vaccination against tetanus.
6. Conclusions
6.1. The necessity of being seen in time
As we can see above, there is a huge part of population suffering from different vision impairments. The fact that our population is getting older with all the age related declines in vision and attention is a real argument for maximum preventive steps including the separation of the bicycle pathways from the motor vehicle traffic.
If a cyclist must use a common space together with the drivers of motor vehicles, he should do a maximum to be seen easily.
In the night, reflexive material can be seen from 3times longer distance than white clothes and from more than 10times longer distance compared to the dark clothes. The light is reflected up to the 200meters. The driver normally needs 1,5 second to realise the danger and react properly. If the motor vehicle moves by the speed of 75km/h, it means minimally 31meters. The reflexive materials give the driver more time to react. By using reflexive clothes, tabs, reflexive bands and other special adds, the visibility and safety of the cyclists on the road can be significantly raised. Intermittent red light has a better effect in attracting the driver’s attention than continually shining red light. It’s highly recommended to use the lights even during daylight within the rush hours (BESIP, 2002). With aging of the population, the speed limits for driving motor vehicles will play more important role in traffic safety.
6.2. Helmets
There are many emotions and side intentions in the topic of wearing a helmet. No helmet can protect a cyclist against the impact with a motor vehicle on the road. This must be solved by a proper separation of cycling routes from the motor vehicle traffic. But there are many statistics proving that every small reduction of the head trauma, even during the impact with the motor vehicle, is of high significance for the condition of injured cyclist. For example Attewell´s meta-analyse of studies collected from several countries published in the period 1987-1998 has summarised odds ratios for efficacy of the helmets for head injury 0.40 (95% confidence interval 0.29, 0.55), for brain injury 0.42 (0.26, 0.67), for facial injury 0.53 (0.39, 0.73) and for fatal injury 0.27 (0.10, 0.71) (Attewell, 2001). If the investigation concentrates on details of cyclist’s condition after collision, the results show that the extent of brain injury and severity of consequences are significantly lower in the cyclists who used a helmet. Depending on the method of study, the reduction in the risk of brain injury as a result of wearing a helmet has been shown to be in the range of 40 % to 85 % all over the world.Safe helmet construction should try to avoid the rotational accelerations that are associated with brain injury and risk to the neck when a helmet catches on the ground or an object and rotates. The safe helmet shell should be as smooth as possible and hard, with fewer openings, round, symmetric, well fixed and fitting on the head (Andersson, 1993; Hansen, 2003). Helmets having a fibre-reinforced plastic (FRP) outer shell absorb energy predominantly by inner shell deformation. Helmets having polycarbonate (PC) thermoplastics outer shells absorb the energy predominantly 'from the outside'. From the aspect of a dangerous head distortion and the risk of an axonal disruption, the well fitting helmet with round smooth FRP shell seems to be a better choice (Beusenberg, 1995). Because statistics showed very low number of impacts on sharp objects in cycling collisions, the hard shells of the cycling helmets are being omitted in favour of lighter and more comfortable helmet constructions.
Padding materials, their strength, amount, shape and its relationship to the head will determine the extent to which the forces generated at impact can be reduced. Padding materials are plastic or elastic. Elastic padding material will recover its original shape and maximum force developed at the impact will be the same and the time when the head is loaded will be doubled. If the helmet must perform its function just once with maximum effect, plastic material is the best (Beusenberg, 1995).
Helmet use had the lowest rate in groups between 11 to 19 years (31%) and 30 to 39 years (30%). The most common reasons given for not wearing a bicycle helmet were: "uncomfortable," "annoying," "it's hot," "don't need it," and "don't own one." Bicycle helmet use was significantly influenced by peer helmet use in all 3 age groups. Children also were more likely to wear a bicycle helmet when their parents or friends wore bicycle helmets (Finnoff, 2001; Gielen, 1994; Sissons, 1994)
Higher rate of wearing cycling helmets was in the cities compared to the country, in cyclists over 50 years of age (Finnoff, 2001) and positively correlated with higher education and better socioeconomic status (Macknin, 1994). These data mostly show the lack of public information and attitude which should be influenced.
Motor vehicle accidents involving cyclists are the most serious cycling collisions, especially for children and seniors. There is therefore a need for improved road engineering methods separating bicycles from other vehicles, traffic calming devices, better education of all road users, as well as helmet and visibility aids usage to improve overall bicycling safety. Every cyclist should know his individual risks and prevention possibilities.
6.3 Cardinal Conclusion
To separate the cyclists from any vehicle transport is the best protection !!!
7. References:
1) Acton CH, Thomas S, Nixon JW, Clark R, Pitt WR, Battistutta D., Children and bicycles: what is really happening? Studies of fatal and non-fatal bicycle injury., PMID: 9346002 MEDLINE, Inj Prev. 1995 Jun;1(2):86-91.
2) Akkermann Kirsti, Harro Jaanus, Käbin Maali, Kiive Evelyn, Platelet monoamine oxidase activity and other markers of monoaminergic systems in predicting impulsivity and risk-taking behaviour, Project of Estonian Science Foundation Research Grant 658882 EEK, 1/1/2003
3) Alušík Štefan et al. (2001), Klinické projevy nežádoucích účinků léků, Triton, Praha 2001, ISBN:80-7254-206-0
4) Anderson Rett, Cerebral Vascular Disease, Stroke, Cerebral Aneurysm, Vascular Disease - Part C, 25th June 2007, MMS Testimonial No. 14 - a Cautionary Note
5) Andersson AL, Bunketorp O.,Cycling and alcohol., Injury. 2002 Jul;33(6):467-71, PMID: 12098540 MEDLINE
6) Attewell RG, Glase K, McFadden M., Bicycle helmet efficacy: a meta-analysis., Accid Anal Prev. 2001 May;33(3):345-52.
7) Aultman-Hall L, Hall FL., Ottawa-Carleton commuter cyclist on- and off-road incident rates., Accid Anal Prev. 1998 Jan;30(1):29-43, PMID: 9542542 MEDLINE,
8) Bečková Ilona, Petr Višňovský, Farmakologie drogových závislsotí, Karolinum 1999, ISBN 80-7184-864-6
9) Berrone S, Gallesio C, Muci G, Amasio M., Relationship between injury dynamics and site of maxillofacial fractures. Comparative study of 100 cases], PMID: 2710083 MEDLINE, Minerva Stomatol.1989 Feb;38(2):161-72.
10) Beusenberg Marc , Riender Happee, Helmet optimization: outer and inner shell behavior with respect to various criteria, International Journal of Injury Control and Safety Promotion, Volume 2, Issue 3 September 1995 , pages 149 - 162
11) Bílová Martina Mgr. et al, Bezpečnost a statistické údaje, bezpečnost cyklistické dopravy - vybrané příklady z ČR a ze zahraničí, Centrum dopraního výzkumu, Konference Národní strategie rozvoje cyklistické dopravy ČR, Velké Karlovice a Slovácko, 15.-19. května 2007
12) Bodtker S, Kramhoft M, Lind J., [Injured cyclists and bicycle passengers. A prospective study of the causes of accidents, accident patterns and consequences], PMID: 2402810 MEDLINE, Ugeskr Laeger. 1990 Aug 20;152(34):2412-5.
13) Braitman, Keli A.1; Kirley, Bevan B.1; Ferguson, Susan2; Chaudhary, Neil K.3, Factors Leading to Older Drivers' Intersection CrashesTraffic Injury Prevention, Volume 8, Number 3, September 2007, pp. 267-274(8), PMID: 17710717 MEDLINE
14) Coeckelbergh TR, Brouwer WH, Cornelissen FW, Kooijman AC., Predicting practical fitness to drive in drivers with visual field defects caused by ocular pathology.,Hum Factors. 2004 Winter;46(4):748-60., PMID: 15709335 MEDLINE
15) Cooke CT, Margolius KA, Cadden GA., Cycling fatalities in Western Australia. PMID: 8264468 MEDLINE, Med J Aust. 1993 Dec 6-20;159(11-12):783-5.
16) Curnow, WJ., The efficacy of bicycle helmets against brain injury, Accident Analysis and Prevention: 2003,35:287-292
17) Cushman R, Down J, MacMillan N, Waclawik H., Bicycle-related injuries: a survey in a pediatric emergency department, CMAJ. 1990 Jul 15;143(2):108-12. PMID: 2364332 MEDLINE
18) Department for Transport - DfT child road safety strategy 2007, UK
19) Departmetn for transport (2004), Road Casualties Great Britain: 2004 Annual Report, Published in September 2005, London: The Stationery Office, ISBN 0-11-522703-6, http://www.dft.gov.uk/pgr/statistics/datatablespublications/accidents/casualtiesgbar/roadcasualtiesgreatbritain2004
20) Dewar Robert E. and Paul L. Olson, 9.1 Our Right to Drive and Our Right to Be Safe: Two Competing Interests, Human Factors in Traffic Safety, 6 1/8" x 9 1/4", casebound, 736 pages. 2004, Lawyers and Judges
21) Drtílková Ivana, Omar Šerý, Hyperkinetická porucha/ ADHD, Galén 2007, pp 268, ISBN 978-80-7262-419-5
22) Finnoff JT, Laskowski ER, Altman KL, Diehl NN (2001). Barriers to bicycle helmet use., Pediatrics. 2001 Jul;108(1):E4.
23) Flegr Jaroslav, Jan Havlícek, Petr Kodym, Marek Malý, Zbyněk Smahel, Increased risk of traffic accidents in subjects with latent toxoplasmosis: a retrospective case-control study, BMC Infectious Diseases 2002, 2:11doi:10.1186/1471-2334-2-11, http://www.biomedcentral.com/1471-2334/2/11
24) Frič Jindřch,Konference nádorní strategie rozvoje cyklsitické dopravy R, kapitola 4, Velké Karlovice a Slovácko, 15. – 19. 5. 2007, Program Besip , Cyklistika a bezpečnost silničního provozu, Ministerstvo dopravy R, odd. BESIP, www.ibesip.cz , jindrich.fric@mdcr.cz;
25) Gilbert K, M McCarthy, Deaths of cyclists in London 1985-92: the hazards of road traffic, BMJ 1994;308:1534-1537 (11 June), http://www.bmj.com/cgi/content/full/308/6943/1535
26) Gorrie C, Duflou J, Brown J, Gibson T, Waite PM., Extent and distribution of vascular brain injury in pediatric road fatalities., J Neurotrauma. 2001 Sep;18(9):849-60., PMID: 11565597 MEDLINE,
27) Hagel BE, Lamy A, Rizkallah JW, Belton KL, Jhangri GS, Cherry N, Rowe BH, The prevalence and reliability of visibility aid and other risk factor data for uninjured cyclists and pedestrians in Edmonton, Alberta, Canada., Accid Anal Prev. 2007 Mar;39(2):284-9, Epub 2006 Oct 4., PMID: 17022929 MEDLINE
28) Haileyesus T, Annest JL, Dellinger AM., Cyclists injured while sharing the road with motor vehicles., Inj Prev. 2007 Jun;13(3):202-6. PMID: 17567979 MEDLINE
29) Hansen KS, Engesaeter LB, Viste A., Protective effect of different types of bicycle helmets, PMID: 14630577MEDLINE, Traffic Inj Prev. 2003 Dec;4(4):285-90.
30) Harisson´s principles of internal medicine, 16th edition, August 2004 / 2,880 pages / 1,148 illustrations, ISBN: 0-07-140235-7
31) Henderson, Michael, Dr., The Effectiveness of Bicycle Helmets: A Review Summary, Revised Edition Prepared by Dr. Michael Henderson, 1995 [Reorder Number MAARE-010995] [ISBN 0 T310 6435 6], http://www.helmets.org/henderso.htm
32) Hermans MH., ConvaTec, Princeton, N.Y., Hydrocolloid dressing versus tulle gauze in the treatment of abrasions in cyclists, PMID: 1797702 MEDLINE, Int J Sports Med. 1991 Dec;12(6):581-4.
33) Herslund MB, Jorgensen NO., Looked-but-failed-to-see-errors in traffic., PMID: 12971922 MEDLINE, Accid Anal Prev. 2003 Nov;35(6):885-91;
34) Hills BL., Vision, visibility, and perception in driving., Perception.1980;9(2):183-216, PMID: 7375327 MEDLINE
35) Himmelreich H, Pralle H, Vogt L, Banzer W., Mountainbike injuries in world-cup and recreational athletes, Sportverletz Sportschaden. 2007 Dec;21(4):180-4.
36) Chow TK, Kronisch RL., Mechanisms of injury in competitive off-road bicycling., Wilderness Environ Med. 2002 Spring;13(1):27-30., PMID: 11929058 MEDLINE
37) Jacobson GA, Blizzard L, Dwyer T., Bicycle injuries: road trauma is not the only concern., Aust N Z J Public Health. 1998 Jun;22(4):451-5. PMID: 9659772 MEDLINE
38) Javouhey E, Guérin AC, Chiron M., UMRESTTE , Incidence and risk factors of severe traumatic brain injury resulting from road accidents: a population-based study., Accid Anal Prev. 2006 Mar;38(2):225-33. Epub 2005 Oct 18.,PMID: 16242108 MEDLINE
39) Jean A. Langlois, Sc.D., M.P.H.,Wesley Rutland-Brown, M.P.H., Karen E. Thomas, M.P.H., Traumatic Brain Injuryin the United States, Emergency Department Visits, Hospitalizations, and Deaths, www.cdc.gov/injury, January 2006
40) Kalita Zbyněk and col. (2006),"Akutní cévní mozkové příhody, Diagnostika, patofyziologie, management", Praha: Maxdorf, 2006, ISBN 80-85912-26-0;
41) Karibe H, Niizuma H, Ohyama H, et al.,Hepatitis C virus (HCV) infection as a risk factor for spontaneous intracerebral hemorrhage: hospital based case-control study. J Clin Neurosci. 2001 Sep; 8(5):423-5.
42) Karkhaneh M, Naghavi M, Rowe BH, Hagel BE, Jafari N, Saunders LD., Changes in the injury pattern of polytraumatized patients over the last 30 years, Unfallchirurg. 2003 Jun;106(6):448-55., PMID: 14567171 MEDLINE
43) Karkhaneha Mohammad,Mohsen Naghavib, Brian H. Rowea, c, Brent E. Hageld, Nahid Jafarib and L. Duncan Saundersa, Epidemiology of bicycle injuries in 13 health divisions, Islamic Republic of Iran 2003, Accident Analysis & Prevention, Volume 40, Issue 1, January 2008, Pages 192-199
44) Kelsch G, Helber MU, Ulrich C.(1996), Craniocerebral trauma in fall from bicycles--what is the effect of a protective helmet?, Unfallchirurg. 1996 Mar;99(3):202-6.PMID: 8685726 MEDLINE
45) Kitchin Jan Lovie et al, Assessment of age-related maculopathy using subjective vision tests, Clin Exp Optom 2005; 88: 5: 292–303
46) Krabbendama Lydia, Pilar Isusib, Paloma Galdosb, Elena Echevarriab, José Ramón Bilbaoc, Ainhoa Martin-Pagolac, Sergi Papiold, Luis Castanoc and Jim Van Osa; Associations between COMTVal158Met polymorphism and cognition: direct or indirect effects?, European PsychiatryVolume 21, Issue 5, July 2006, Pages 338-342, doi:10.1016/j.eurpsy.2006.03.007
47) Kurzthaler I, Wambacher M, Golser K, Sperner G, Sperner-Unterweger B, Haidekker A, Pavlic M, Kemmler G, Fleischhacker WW. Alcohol and/or benzodiazepine use in injured road users., PMID: 12858322 MEDLINE, Hum Psychopharmacol. 2003 Jul;18(5):361-7;
48) Larsen L V, The epidemiology of bicyclists collision accidents, Journal of Traffic Medicine, 22:27-31, 1994.
49) Lindqvist C, Sorsa S, Hyrkäs T, Santavirta S., Maxillofacial fractures sustained in bicycle accidents., Int J Oral Maxillofac Surg. 1986 Feb;15(1):12-8.
50) Macknin M. L. and S. V. Medendorp, Association between bicycle helmet legislation, bicycle safety education, and use of bicycle helmets in children, Archives of Pediatrics & Adolescent Medicine JAMA & Archives Vol. 148 No. 3, March 1994
51) Maimaris C, Summers CL, Browning C, Palmer CR., Injury patterns in cyclists attending an accident and emergency department: a comparison of helmet wearers and non-wearers., BMJ. 1994 Jun 11;308(6943):1537-40, PMID: 8019309
52) Marinella, Často přehlédnuté diagnózy v akutní péči, Grada, 2007, ISBN 978-80-247-1735-7
53) Martin JL, Lafont S, Chiron M, Gadegbeku B, Laumon B., Differences between males and females in traffic accident risk in France, PMID: 15480293 MEDLINE, Rev Epidemiol Sante Publique. 2004 Sep;52(4):357-67.
54) McGarry Teresa and Rob Sheldon, Accent February 2008, Department for Transport: London, Road Safety Research Report No. 84, Cycle Helmet Wearing in 2006, http://www.dft.gov.uk/pgr/roadsafety/research/rsrr/theme1/cyclehelmets.pdf
55) McLennan JG, McLennan JC, Ungersma J., Accident prevention in competitive cycling., Am J Sports Med. 1988 May-Jun;16(3):266-8.
56) Mraček J., Choc M., Cyklistické úrazy z pohledu neurochirurga, Prakt. Lék., 2004, 84, No. 9, p. 506-509.
57) Mravcík V, Vorel F, Zábranský T., Drugs and fatal traffic accidents in the Czech Republic., PMID: 18251231 MEDLINE, Cent Eur J Public Health. 2007 Dec;15(4):158-62.
58) National center for Injury Prevention and Control, Traumatic Brain Injury, http://www.cdc.gov/ncipc/factsheets/tbi.htm
59) Neklapil Ondřej, Kapitola z bakalářské práce z Policejní Akademie České republiky v Praze, Katedra bezpe nostních služeb (duben 2007), Konference nádorní strategie rozvoje cyklsitické dopravy, Velké Karlovice a Slovácko, 15. – 19. 5. 2007
60) Nelson Sara W., MD; Daniel M. Lindberg MD, The Unrestrained Driver, Release Date: March 28, 2008; Valid for credit through March 28, 2009, e-medicine casustics of the week at: http://em.emedicine.com/cgi-bin1/DM/y/eBjI60UT8bw0WMy0JJMS0Ej
61) Nixon J, Clacher R, Pearn J, Corcoran A.(1987), Bicycle accidents in childhood.,PMID: 3109611 MEDLINE, Br Med J (Clin Res Ed). 1987 May 16; 294(6582): 1267–1269. PMCID: PMC1246435
62) Ondráček Jan , Ph. D., Mgr. Sylva Hřebíčková, Úkol 1. Bezpečnost provozování cykloturistiky, FSpS MU Brno, tech. spolupráce: Servisní středisko pro podporu e-elarningu na MU, Brno 2006, http://is.muni.cz/elportal/estud/fsps/js07/turistika/ch01s01.html
63) Owsley C, Ball K, Sloane ME, Roenker DL, Bruni JR.(1991), Visual/cognitive correlates of vehicle accidents in older drivers., Psychol Aging. 1991 Sep;6(3):403-15.,PMID: 1930757 MEDLINE
64) Parslow , K P Morris, R C Tasker, R J Forsyth, C A Hawley,Epidemiology of traumatic brain injury in children receiving intensive care in the UK,Published Online First: 27 July 2005. doi:10.1136/adc.2005.072405, Archives of Disease in Childhood 2005;90:1182-1187
65) Pasanen Eero, The risks of cycling, Helsinki City Planning Department, Traffic Planning Division, Aleksanterinkatu 26, HELSINKI, FINLAND, 2003
66) Pokorný Petr, Ing.(2007), Bezpečnost a statistické údaje, cyklistika - rizika (překlad), Centrum dopravního výzkumu, Konference národní srategie rozvoje cyklsitické dopravy R, kapitola 4,Velké Karlovice a Slovácko, 15. – 19. 5. 2007, www.cdv.cz
67) Preidt Robert, Smoking Boosts 'Bleeding' Stroke Risk in Those With High Blood Pressure, SOURCE: American Heart Association, news release, March 6, 2008http://www.lex18.com/Global/story.asp?S=7977673
68) příloha č. 13 k vyhlášce č. 341/2002 Sb.
69) Puranik S, Long J, Coffman S., Profile of pediatric bicycle injuries., PMID: 9824185 MEDLINE, South Med J. 1998 Nov;91(11):1033-7.
70) Räsänen M, Summala H., Attention and expectation problems in bicycle-car collisions: an in-depth study period of 1991-1997, PMID: 9678219 MEDLINE, Accident Analysis and Prevention, Volume 30, Number 5, September 1998 , pp. 657-666(10), Publisher: Elsevier, Accid Anal Prev. 2001 Mar ;33 (2):187-96 11204889 (P,S,E,B),
71) Reimera Bryan, Lisa A. D’Ambrosioa, Jennifer Gilberta, Joseph F. Coughlina, Joseph Biedermana, Craig Surmanb, Ronna Friedb and Megan Aleardib; Behavior differences in drivers with attention deficit hyperactivity disorder: The driving behavior questionnaire, Accident Analysis & Prevention, Volume 37, Issue 6, November 2005, Pages 996-1004, doi:10.1016/j.aap.2005.05.002
72) Rivara FP, Astley SJ, Clarren SK, Thompson DC, Thompson RS., Fit of bicycle safety helmets and risk of head injuries in children., PMID: 10518266 MEDLINE, Inj Prev. 1999 Sep;5(3):194-7
73) Rivara FP, Thompson DC, Thompson RS., Epidemiology of bicycle injuries and risk factors for serious injury, Inj Prev. 1997 Jun;3(2):110-4, PMID: 9213156 MEDLINE
74) Rivara, D. C. Thompson and R. S. Thompson, Epidemiology of bicycle injuries and risk factors for serious injury, Injury Prevention, Vol 3, Issue 2, pp 110-114
75) Sgaglione NA, Suljaga-Petchel K, Frankel VH. (1982), Bicycle-related accidents and injuries in a population of urban cyclists., Orthop Inst. 1982 Spring;42(1):80-91, PMID: 6288156 MEDLINE
76) Sharples PM, Storey A, Aynsley-Green A, Eyre JA., Causes of fatal childhood accidents involving head injury in northern region, 1979-86., BMJ. 1990 Nov 24;301(6762):1193-7, PMID: 2261557 MEDLINE
77) Shepard Scott, Editor(s): Scott C Dulebohn, Paolo Zamboni, John Geibel, Head Trauma, Last Updated: August 20, 2004, http://www.emedicine.com/med/TOPIC2820.HTM
78) Schoon, Nehody jízdního kola bez spoluzavinění jiným ú astníkem provozu, Konference národní srategie rozvoje cyklsitické dopravy R, kapitola 4,Velké Karlovice a Slovácko, 15. – 19. 5. 2007
79) Slootmans FC, Biert J, de Waard JW, de Waal Malefijt MC, Schoots FJ., Femoral neck fractures in bicyclists due to clipless pedals, Ned Tijdschr Geneeskd. 1995 Jun 3;139(22):1141-3., PMID: 7791912 MEDLINE
80) Soori H, Bhopal RS., Parental permission for children's independent outdoor activities. Implications for injury prevention, Eur J Public Health, 2002 Jun;12(2):104-9.
81) Summala H.; Pasanen E.; Rasanen M.; Sievanen J., Bicycle accidents and drivers' visual search at left and right turns, Accident Analysis and Prevention, Volume 28, Number 2, March 1996 , pp. 147-153(7), Publisher: Elsevier
82) Šerý, Omar - Novák, Lubomír - Izakovičová Hollá, Lydie - Štastný, František - Jirák, Roman - Zeman, Miroslav - Kaňková, Kateřina - Zikán, Michal - Pavlišta, David - Lochman, Jan - Kovář, Vratislav - Řezníček, Vít - Maňasková, Dana, Vybrané přednášky z prediktivní genetiky. první vydání. Praha : Ing. Jiří Rotschedl, 2007. 74 s. 1. svazek. ISBN 978-80-903367-3-5;
83) Šerý, Omar - LOCHMAN, Jan - ZVOLSKÝ, Petr - HLINOMAZOVÁ, Zuzana (2008). Porucha barvocitu u alkoholiků a její souvislost s polymorfizmem genu pro BDNF. Česká a slovenská psychiatrie, Praha, Česká lékařská společnost J.E. Purkyně. ISSN 1212-0383, 2008
84) The National Highway Traffic Safety Administration (205), USA, http://www.nhtsa.dot.gov/portal/site/nhtsa/menuitem.cc7fa94f0c9b3dd24ec86e10dba046a0/
85) Thompson DC, Rivara FP, Thompson R., Helmets for preventing head and facial injuries in bicyclists. PMID: 10796827 MEDLINE, Cochrane Database Syst Rev. 2000;(2):CD001855.
86) Topinková Eva, Geriatrie pro praxi, 1. vydání, Vydavatelství Galen, 2005, ISBN 80-7262-365-6
87) Towner Elizabeth, Therese Dowswell, Matthew Burkes, Heather Dickinson, John Towner, Michael Hayes, Bicycle helmets: review of effectiveness (No.30), November 2002, http://www.dft.gov.uk/pgr/roadsafety/research/rsrr/theme1/bicyclehelmetsreviewofeffect4726?page=12
88) Valent Francesca, D’Anna Little, Giorgio Tamburlini, Fabio Barbone, Environmental Burden of Disease Series, No. 8, Burden of disease attributable to selected environmental factors and injuries among Europe's children and adolescents, ISBN 92 4 159190 0 http://www.who.int/quantifying_ehimpacts/publications/en/ebd8web.pdf
89) Vorel František and col., "Soudní lékařství", 1st printing, Praha: Grada, 1999, pp.606, ISBN 80-7169-728-1
90) Wheatley J, Cass DT. (1989), Traumatic deaths in children: the importance of prevention., Med J Aust. 1989 Jan 16;150(2):72-8.
91) Wilson Mighk, Bicycle & Pedestrian Coordinator, Orlando Area Bicyclist Crash Study: A Role-Based Approach to Crash Countermeasures A Study of Bicyclist-Motorist Crashes in the Orlando Urban Area in 2003 and 2005, FL 32801-1949, 407-481-5672 ext. 318, www.metroplanorlando.com
92) Zagaria Mary Ann E., Vision, Cognition, and Mobility Challenges for Elderly Drivers, US Pharm. 2007;1:36-40. Vol. No: 32:01, http://www.uspharmacist.com/index.asp?show=article&page=8_1932.htm
93) Zidan Abu, Nagelkerke N, Rao S., Factors affecting severity of bicycle-related injuries: The role of helmets in preventing head injuries, PMID: 17655641 MEDLINE, Emergency Medicine Australasia, Volume 19, Number 4, August 2007, pp. 366-371(6), Blackwell Publishing;